Research Team Create First 3D/4D “Whole-Brain Map” for Neurosurgery Patients
 After ten years of continuous work, a combined Children’s Hospital of Michigan and Wayne State University School of Medicine (WSUSOM) research team has successfully developed a set of electronic tools that can draw “space and time-based” maps of the neuron-signaling across speech and language centers of the human brain.
After ten years of continuous work, a combined Children’s Hospital of Michigan and Wayne State University School of Medicine (WSUSOM) research team has successfully developed a set of electronic tools that can draw “space and time-based” maps of the neuron-signaling across speech and language centers of the human brain.
The whole-brain level 3D and 4D-mapping techniques represent a significant breakthrough in the effort to prevent both pediatric and adult patients who struggle with epilepsy or tumors from experiencing “speech and language deficits” that can result from corrective surgery performed in those areas of the brain.
Led by the Children’s Hospital of Michigan Director of Neurodiagnostics and WSUSOM pediatric neurology researcher Eishi Asano, MD, PhD, MS (CRDSA), the breakthrough study was published March 16, 2017 in Brain, a leading international scientific journal based in the UK.
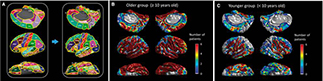 “This is believed to be the first time that neurology researchers have ever been able to look at the origin and propagation of electro-signaling related to speech and language centers at the whole-brain level at a temporal resolution of 1/100 seconds, and our 4D map will ultimately improve the quality of life in patients undergoing surgery designed to reduce epileptic seizures or remove brain tumors,” said Dr. Asano, a 20-year-veteran pediatric neurologist at the Children’s Hospital of Michigan.
“This is believed to be the first time that neurology researchers have ever been able to look at the origin and propagation of electro-signaling related to speech and language centers at the whole-brain level at a temporal resolution of 1/100 seconds, and our 4D map will ultimately improve the quality of life in patients undergoing surgery designed to reduce epileptic seizures or remove brain tumors,” said Dr. Asano, a 20-year-veteran pediatric neurologist at the Children’s Hospital of Michigan.
“The first comprehensive human brain map, originally hand drawn in a 2D manner by Wilder G. Penfield and his colleagues in Montreal Neurological Institute in 1937, still serves as important textbook materials for current students in medicine, psychology, and neuroscience,” said Dr. Asano. “During the last decade, a number of investigators generated 3D maps of speech and language, using functional imaging techniques measuring blood flow changes, but such conventional techniques are unable to delineate the rapid dynamics of brain activation and deactivation taking place in the order of tens of milliseconds. Our study successfully added a timing dimension to the 3D brain surface image, by measuring high-frequency electrographic activity directly from the brain surface during the surgical evaluation. Our 4D whole-brain level map is a breakthrough discovery with the potential to improve outcomes for epilepsy and tumor patients, both pediatric and adult.”
The ten-year study examined electro-signaling activity in 100 patients whose brain-based speech and language centers were “mapped” with the newly developed high-tech tool. This technique is child-friendly and readily applicable to young children who may not be too cooperative to undergo conventional mapping examinations.
“The bottom line is this new 3D and 4D-mapping technology will significantly reduce the risk of language deficits after surgery to reduce epileptic seizures or remove brain tumors. For both pediatric and adult patients, avoiding such deficits following brain surgery is extremely important for quality of life, and we are greatly encouraged by the potential improvements in patient care that could emerge from the use of this new electrophysiology/imaging fusion process,” said Dr. Asano.
The recently published study in Brain also noted the potential benefits for patients at given ages, while pointing out: “This 4D brain mapping technique can further improve the understanding of the developmental ontogeny of cortical network dynamics responsible for speech and language processing from infancy to adulthood.”
Dr. Asano was also careful to credit his “outstanding collaborators” for their part in the project.
“This study has been a collaborative effort from the very beginning,” said Dr. Asano “and the research couldn’t have occurred without the continuing dedication and innovative skills of the entire team.
“I am particularly grateful to Pediatric Neurosurgeon Sandeep Sood, MD, Neuropsychologist Robert Rothermel, PhD, at the Children’s Hospital of Michigan, for their insights and experience and continuing determination to see the project through. Such teamwork is the key to achieving results that can bring better healthcare to patients, and the researchers at both the Children’s Hospital of Michigan and the Wayne State University School of Medicine have distinguished themselves in the effort to successfully develop these exciting new brain-mapping tools.”
The Children’s Hospital of Michigan Chief of Pediatric Neurology Dr. Lalitha Sivaswamy said, “These new brain mapping tools offer a great deal of promise to pediatric patients who struggle with epilepsy and brain tumors. Dr. Asano and his colleagues are certainly to be congratulated for the immense amount of work and energy that has gone into this research. It’s no accident that their work is now being recognized by one of the world’s great scientific journals as an important breakthrough. Making life easier – and healthier – for patients who receive surgical therapy is a vitally important goal for all of us in pediatric medicine, and it’s wonderfully encouraging to see that work now going forward in a world-class publication such as Brain.”



.png?sfvrsn=553ab186_0)

.jpg?Status=Master&sfvrsn=d1560cec_0)