Children’s Hospital of Michigan Launches First Neuro-Neonatal Intensive Care Unit in the State
 In order to address the significant need to manage and minimize neurological complications associated with preterm and term newborn babies, Children’s Hospital of Michigan is pleased to announce its newly developed Neuro-Neonatal Intensive Care Unit (NeuroNICU).
In order to address the significant need to manage and minimize neurological complications associated with preterm and term newborn babies, Children’s Hospital of Michigan is pleased to announce its newly developed Neuro-Neonatal Intensive Care Unit (NeuroNICU).
Children’s Hospital of Michigan’s NeuroNICU is the first-of-its-kind in the state of Michigan and one of a select few across the nation. This program offers a specially trained team of clinicians dedicated to providing an appropriate environment that will help optimize neurologic and developmental outcomes for this highly vulnerable population.
 “We are excited to join other select premier children’s hospitals throughout the country in establishing the NeuroNICU program,” said Girija Natarajan, M.D., Co-Chief Division of Neonatology, Clinical Operations and Education at Children’s Hospital of Michigan and Hutzel Women’s Hospital. “This program is aimed at ensuring preterm and term newborns at risk for brain injury and future developmental problems are meticulously cared for by a team of specialists.”
“We are excited to join other select premier children’s hospitals throughout the country in establishing the NeuroNICU program,” said Girija Natarajan, M.D., Co-Chief Division of Neonatology, Clinical Operations and Education at Children’s Hospital of Michigan and Hutzel Women’s Hospital. “This program is aimed at ensuring preterm and term newborns at risk for brain injury and future developmental problems are meticulously cared for by a team of specialists.”
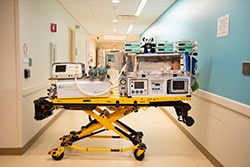
The NeuroNICU offers a six-bed unit housed within part of the newly expanded and renovated single room Neonatal Intensive Care Unit (NICU) on the third floor of the Children's Hospital of Michigan Tower. The program will offer key pillars of care including neurological assessments, diagnostics, neuro-protection therapies and advancements in neurodevolopmental care. Transport cooling by the Tecotherm device with the dedicated pediatric and neonatal transport team (PANDA) will allow infants with birth asphyxia to be started early with cooling and be transported to the NeuroNICU at Children’s Hospital of Michigan. The program will also provide prevention and treatment of neonatal brain hemorrhage and its complications among extremely low gestational age neonates. The program is a collaborative effort between neonatologists, pediatric neurologists and neurosurgeons, pediatric neuroradiologists, neonatal nurses with special interest in brain injury, EEG technologists, psychologists, occupational therapists, physical therapists, dietitians and social workers.
 After the patient is released from the NeuroNICU, continuum of care includes a multidisciplinary developmental assessment clinic where all neonatal neurocritical care patients will be followed for five years. Collective care includes specialists from physical medicine and rehabilitation, neonatology and neuropsychology.
After the patient is released from the NeuroNICU, continuum of care includes a multidisciplinary developmental assessment clinic where all neonatal neurocritical care patients will be followed for five years. Collective care includes specialists from physical medicine and rehabilitation, neonatology and neuropsychology.
“As the state’s first and oldest pediatric hospital, Children’s Hospital of Michigan has always been dedicated to treating the most vulnerable – this NeuroNICU program was created specifically for them,” said Luanne Thomas Ewald, CEO of Children’s Hospital of Michigan. “Our hospital is at the forefront of research on neurological protection, preservation and treatment and with the increasing survival rate of NICU patients, there is a greater need to focus on improving neurodevelopment among high-risk survivors.”
The NICU at Children’s Hospital of Michigan is a Level IV NICU, offering the highest degree of care for premature or critically ill newborns. It is a regional referral center for advanced neonatal therapies, such as extracorporeal membrane oxygenation, high-frequency ventilation, advanced neonatal neuroimaging, and therapeutic hypothermia, or for coordination of complex care requiring multiple types of pediatric specialists only available at a children’s hospital.
“The opening of this state-of-art neonatal care program will greatly enhance the research capabilities of Children’s Hospital of Michigan and elevate its position as a premier center for research trials in neonates in the state and the country,” said Seetha Shankaran, M.D., neonatologist at Children’s Hospital of Michigan and Hutzel Women’s Hospital and principal investigator for the first randomized controlled trial conducted by NICHD Neonatal Research Network on whole body cooling for hypoxic-ischemic encephalopathy. The significant benefits of cooling in reducing death or disability shown by the trial she led established cooling as standard of care throughout the world. “We are able to offer innovative care for newborns with neurological needs; stem cells are a recent example. This addition of the NeuroNICU program to Children’s Hospital of Michigan will surely advance the standard of prenatal care for our city.”
To consult with a NeuroNICU expert or to transfer a patient to Children’s Hospital of Michigan, call the Physician Link Line at 1-877-994-8436. For more information, visit childrensdmc.org/NeuroNICU.



.png?sfvrsn=553ab186_0)

.jpg?Status=Master&sfvrsn=d1560cec_0)