What is a corpus callosotomy?
Corpus callosotomy is a surgical procedure used to treat atonic seizures, also called drop attacks, by dividing all or part of the corpus callosum. The corpus callosum is the bundle of nerve fibers that connects the two brain hemispheres. The procedure
prevents seizures from spreading from one half of the brain to the other. Corpus callosotomy surgery does not completely eliminate seizures, but it prevents them from affecting the entire brain and muscles on both sides of the body.
How is corpus callosotomy surgery performed?
Corpus callosotomy surgery is performed while your child is under general anesthesia.
Two methods are used for the procedure.
- Conventional method: A small incision is made in the scalp at the top of the head, and a section of the skull is removed. The neurosurgeon gently separates the two hemispheres and uses special instruments and surgical microscopes to disconnect the
corpus callosum or to cut part of it. The section of skull removed at the start of the procedure is then replaced and fixed in position, and the skin incision is closed.
- Laser ablation brain surgery: Two to three small holes are made in the skull and the laser surgery is guided by magnetic resonance imaging (MRI). Heat from the precisely focused laser beam cuts the corpus callosum. Nearby brain tissue is not affected,
and no brain tissue is touched or moved to gain access to the corpus callosum.
What are some of the benefits of a laser ablation brain surgery?
Robotic neurosurgery offers a simplified, precise, and safe alternative for extra-operative invasive evaluation, and is particularly well-suited for deep-seated/difficult to cover locations, failures of previous subdural invasive studies, extensive bi-hemispheric
explorations, and pre-surgical evaluation suggestive of a functional network involvement.
This minimally invasive approach allows patients to avoid an invasive craniotomy, allowing:
- Shorter operating time
- Faster recovery time from procedure
- Fewer complications
What is ROSA?
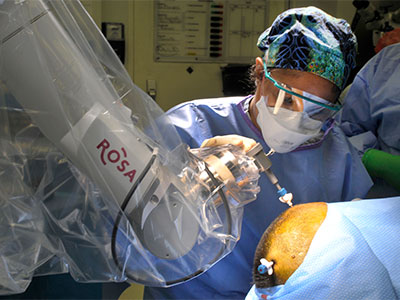
ROSA is a surgical navigation and positioning system using robotic technology that allows surgeons to place instruments in the brain without having to open a patient’s skull or even shave a patient’s head, as other traditional methods require.
The ROSA system is used to support many neurosurgical procedures, including stereoelectroencephalography (SEEG), thermal ablation of seizure foci or tumors, deep brain stimulation (DBS) and surgical treatment of movement disorders.
The surgeon uses ROSA and its planning software to create a 3D map of the patient’s brain and plan out exact pathways needed to carry out the procedure. ROSA Brain is aligned to the trajectories outlined by the surgical plan, and the surgeon carries
out the surgery utilizing the robot as a guide. ROSA Brain provides robotic alignment of the planned pathway which allows the surgeon to reach a deep brain target for the placement of surgical instruments.